Home › Forums › Oral Diagnosis & Medicine › TREATMENT FOR LICHEN PLANUS
Welcome Dear Guest
To create a new topic please register on the forums. For help contact : discussdentistry@hotmail.com
- This topic has 3 replies, 1 voice, and was last updated 23/04/2012 at 5:23 pm by
Drsumitra.
-
AuthorPosts
-
23/04/2012 at 5:21 pm #15420
Drsumitra
OfflineRegistered On: 06/10/2011Topics: 238Replies: 542Has thanked: 0 timesBeen thanked: 0 times23/04/2012 at 5:22 pm #15421Drsumitra
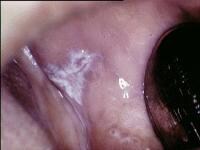
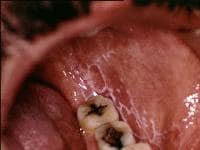
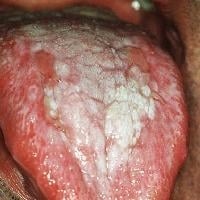
OfflineRegistered On: 06/10/2011Topics: 238Replies: 542Has thanked: 0 timesBeen thanked: 0 timesCurrent data suggest that oral lichen planus is a T-cell–mediated autoimmune disease in which autocytotoxic CD8+ T cells trigger apoptosis of oral epithelial cells.[1, 2]
The dense sub-epithelial mononuclear infiltrate in oral lichen planus is composed of T cells and macrophages, and there are increased numbers of intra-epithelial T cells. Most T cells in the epithelium and adjacent to the damaged basal keratinocytes are activated CD8+ lymphocytes. Therefore, early in the formation of oral lichen planus lesions, CD8+ T cells may recognize an antigen associated with the major histocompatibility complex (MHC) class I on keratinocytes. After antigen recognition and activation, CD8+ cytotoxic T cells may trigger keratinocyte apoptosis. Activated CD8+ T cells (and possibly keratinocytes) may release cytokines that attract additional lymphocytes into the developing lesion.[2]
Oral lichen planus lesions contain increased levels of the cytokine tumor necrosis factor (TNF)–alpha.[3, 4] Basal keratinocytes and T cells in the subepithelial infiltrate express TNF in situ.[5, 6] Keratinocytes and lymphocytes in cutaneous lichen planus express elevated levels of the p55 TNF receptor, TNF-RI.[7] T cells in oral lichen planus contain mRNA for TNF and secrete TNF in vitro.[8] Serum and salivary TNF levels are elevated in oral lichen planus patients.[9, 10, 11, 12] TNF polymorphisms have been identified in patients with oral lichen planus, and they may contribute to the development of additional cutaneous lesions.[13] Oral lichen planus has been treated successfully with thalidomide,[14, 15] , while thalidomide is known to suppress TNF production.[16, 17] Together, these data implicate TNF in the pathogenesis of oral lichen planus.
The lichen planus antigen is unknown, although it may be a self-peptide (or altered self-peptide), in which case lichen planus would be a true autoimmune disease. The role of autoimmunity in the pathogenesis is supported by many autoimmune features of oral lichen planus, including its chronicity, onset in adults, predilection for females, association with other autoimmune diseases, occasional tissue-type associations, depressed immune suppressor activity in patients with oral lichen planus, and the presence of autocytotoxic T-cell clones in lichen planus lesions. The expression or unmasking of the lichen planus antigen may be induced by drugs (lichenoid drug reaction), contact allergens in dental restorative materials or toothpastes (contact hypersensitivity reaction), mechanical trauma (Koebner phenomenon), viral infection, or other unidentified agents.
23/04/2012 at 5:23 pm #15422Drsumitra
OfflineRegistered On: 06/10/2011Topics: 238Replies: 542Has thanked: 0 timesBeen thanked: 0 timesRe-examine patients with oral lichen planus (OLP) during active treatment, and monitor lesions for reduction in mucosal erythema and ulceration and alleviation of symptoms. Continue active treatment and try alternative therapies until erythema, ulceration, and symptoms are controlled. Follow up with patients with oral lichen planus at least every 6 months.
Advise patients with oral lichen planus to pay attention to when symptoms are exacerbated or when lesions change. Such changes generally indicate a phase of increased erythematous or erosive disease.
In view of the potential association of oral lichen planus with oral SCC, an appropriate specialist should follow up with the patients every 6-12 months. In addition, advise patients to regularly examine their mouths and seek the help of a specialist if persistent red or ulcerative oral mucosal lesions develop.
Candidal cultures or smears may be obtained periodically. Infections can be controlled with topical antimycotic preparations. These tests may be of limited clinical value because oral C albicans is present in at least 70% of all healthy persons.
-
AuthorPosts
- You must be logged in to reply to this topic.